Robotic Surgery at Center for Prostate Cancer NYC
- Before Your Surgery
- After Your Surgery
- Continence After Surgery
- Sexual Function After Prostate Surgery
At the Center for Prostate Cancer NYC, our Precision Urology™ approach involves integration of multiple variables and imaging data in a decision-support system.
For us, each case is special, and we are committed to personalizing care for each patient. We understand your fears, challenges, and hopes, and we will be with you through your journey of recovery from prostate cancer.

Dr. Tewari and his team are among the most skilled, sought after, appreciated, and caring teams in the U.S.
We are passionate about researching, selecting, delivering, and monitoring the right treatment for you. Read about the options and techniques used by Dr. Tewari and his team to provide the best solution for your prostate cancer.

Precautions around Medications
Certain medications may interfere with the clotting and coagulation of the blood and can increase the risk of bleeding before and after surgery. To avoid this risk, we advise you to consult your prescribing physician(s) and with their approval to stop taking the following medications 30 days prior to your surgery:
- Aspirin
- Non-steroidal anti-inflammatory drugs (e.g., Motrin, Advil, Celebrex, and Arthotec)
- Vitamin E, fish oil, fax seed oil, and all supplements
- Plavix
We also recommend that you stop taking Coumadin seven days prior to surgery, with the permission of your prescribing doctor.
Procuring Medical Clearance
We advise you to obtain a medical clearance from your primary care physician in advance of your surgery to confirm you are strong enough for the robotic procedure. If you do not have a primary care physician, we can recommend one for you.

Pre-Admission Tests
Prior to your appointment, you will be asked to gather certain medical information pertinent to your general health and any information you may have related to your prostate cancer diagnosis.
Typically these are:
- PSA and general blood test results
- prostate biopsy slides
- pathology reports
- imaging results
We will be happy to answer any questions you may have about getting your clinical information together at the time we schedule your evaluation appointment. You may be asked to undergo further testing after your initial visit.
During your initial prostate cancer evaluation visit, you will be examined by Dr. Tewari and members of his clinical team who will also review your clinical records. Your suitability for ARTTM robotic prostate surgery will be evaluated and discussed with you. You will have ample opportunity to discuss any concerns and to ask any questions you may have.
If you are a suitable prostate cancer surgery candidate and you wish to schedule the surgery, you may begin that process right after you have been evaluated. Alternatively, you may wish to take time to consider the decision and to contact us at a later date to schedule your robotic surgery.

Insurance Information
If you decide to proceed with ARTTM robotic surgery, you will be asked to provide us with your insurance information, if applicable. Our financial counselors will discuss payment options with you and are ready to assist you with banking and fund transfers, currency conversions, and verification of insurance benefits, if appropriate. We will provide you with an estimate of charges for physician and hospital services, as well as arrange for pre-admission deposits and special packages.
If you do not have insurance coverage you will be responsible for all charges related to your surgery. Payment arrangements will be discussed with you at the time your surgery is scheduled.
Maintaining Physical Activity
We recommend that you do moderate exercise and activity before surgery to promote faster healing.
- If you are already exercising regularly, you should maintain a moderate level of exercise prior to surgery.
- If your lifestyle is more sedentary, we recommend that you begin walking one to two miles daily to prepare your body.
After surgery you will be in “Prostate Bootcamp” and we will ask you to walk up to three miles daily. This exercise will be easier if you are already walking regularly. (In addition, “Prostate Bootcamp” requires drinking eight to 12 glasses of water daily for one month after surgery.)

The Day Before Surgery
The day before surgery, our team will guide you in making certain dietary and bowel preparations:
- Drink one bottle (10 ounces) of magnesium citrate in the morning (magnesium citrate is available at most pharmacies)
- Take one Fleet enema in the evening
We advise you to drink plenty of fluids throughout the day as the bowel prep will make you lose fluid. You should stop eating or drinking by midnight.

Blood Banking
Blood loss during robotic surgery is minimal, so we do not ask you to donate your own blood before the procedure. If you would like to do so, we can make these arrangements for you. You will need to donate no more than two units three to four weeks before the surgery.
Banking Sperm
After the robotic prostatectomy, you should continue to have normal desire and orgasm. Whether you will have an erection is a somewhat more complicated question and depends on several factors, such as the stage of your cancer and the strength of your erections before surgery.
Dr. Tewari’s ART™ surgery technique is designed to eradicate the cancer while minimizing damage to the nerves responsible for erectile function. Most patients do regain the ability to have erections, but this is a gradual process and can take up to a year (or more), with erections usually improving over time.
However, after the prostatectomy, you will no longer be able to ejaculate. This is because we will have removed the prostate and seminal vesicle, which produce most of the seminal fluid. Men who have had a prostatectomy are not able to father children. If you are considering the possibility of fathering children in the future, banking sperm is an option. The cost is covered by most insurance companies.
After Your Surgery: 24 hours after the procedure
- You will be transferred to your room after your surgery. You will have six small bandages over the skin incisions, a drain on one side of your abdomen attached to a vacuum container, and a urine catheter (Foley) to drain urine from your bladder. The Foley catheter will be attached to a urine bag. An intravenous (IV) line will deliver fluids to your body. The IV and drain are usually discontinued the day after surgery.
- You will be allowed to have ice chips and sips of water. Pain is generally minimal, but pain medication will be administered, if necessary.
- The key to fast recovery and return to normal bowel activity is early walking. Once you are ready, you should sit up and attempt to walk a few steps. Walking also improves blood circulation in the legs and prevents clot formation.
- The next morning, you may have a light breakfast and a liquid diet thereafter. You may not have solid food until you pass intestinal gas and have a bowel movement. Most people do not pass intestinal gas for several days and do not have a bowel movement for three to four days.
- Your major contribution to your speedy recovery comes on the day after surgery, when you are expected to walk in the hallways a total of one mile, or 25 laps around the hospital wing (but not in one grand sprint).
- You will also be given a breathing device, called a spirometer. Using it will help expand your lungs and prevent infections. You should use this device once every hour and take 10 consecutive deep breaths with the spirometer in your mouth.
Most of Dr. Tewari's robotic prostatectomy patients are discharged and return home the day after surgery.

After Your Surgery: Urine Catheter
When you leave the hospital, the urinary catheter will remain in place.
- The catheter will remain in place for approximately six to nine days after the surgery. The catheter will be attached to a leg bag that you can hide under your trousers. At night, we recommend that you switch to a regular urinary bag that you place on the side of the bed. This is a larger bag that will allow you to sleep through the night without the need to get up to use the toilet.
- You may experience some bladder pain or cramps (spasms) associated with the catheter, but most people tolerate the catheter well. You may also leak minimal amounts of urine around the catheter because of involuntary bladder contractions. You may want to wear a pull-up diaper over the catheter to prevent soiling your clothing.
- It is also not unusual to notice pink or red tinged urine after a walk or bowel movement. Do not be alarmed. Simply increase your fluid intake until the urine becomes clear again and lie down for some time. All of these events are considered within normal range and you should not be concerned.
Most of Dr. Tewari's robotic prostatectomy patients are discharged and return home the day after surgery.

After Your Surgery: Catheter Removal
On the day of your scheduled catheter removal, you will come to the hospital to have a cystogram (this is only required if Dr. Tewari requests it). To perform a cystogram, a radiologist injects dye through the catheter and takes an x-ray to make sure that there is no leakage at the point where the bladder and urethra connect.
You will then come to Dr. Tewari's office for removal of the catheter (a relatively pain-free procedure). After the catheter is removed, most men cannot control the urine sphincter and leak urine for a few days to weeks. While we encourage patients to bring diapers and protective pads with them the day of the catheter removal, many patients stop leaking within a few hours or days.
A minority of patients (five percent) may have delayed healing of the bladder/urethra connection and thus require longer catheterization or may require re-insertion of the catheter because of swelling at the connection.
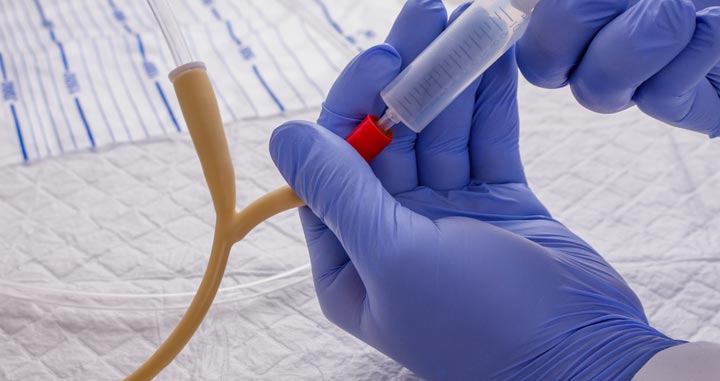
After Your Surgery : Activity
Travel/Driving:
You can return home by car from the hospital after discharge if your drive is within two hours, but you should not drive for two weeks. If you come from out of state and are traveling by plane, make sure that you walk every half hour in the plane cabin to prevent blood clotting in the legs.
Physical Activity:
It takes three to four weeks for the abdominal incisions to heal completely, so you should avoid heavy lifting during that time. You may have some swelling in the scrotum and penis after surgery, which will resolve with time. If this occurs, elevate your scrotum using a folded towel when you lie down, and wear mildly tight underpants when you move about.
You can shower any time after surgery, but do not take a bath until after the urine catheter is removed. Leave the bandages on the skin incisions for three to four days.
Returning to Normal Routines:
You can start your daily activities (such as walking, climbing stairs, etc.) immediately when you get home. However, you should wait three to four weeks before beginning any heavy exercise, such as jogging, weightlifting, and bicycle riding. Generally, you can return to work two to three weeks after the surgery depending on the type of work you do.

Continence After Your Prostate Robotics Surgery
Dr. Tewari and his team of clinicians and researchers have won awards for advancing the field of nerve-sparing prostate surgery. During surgery, Dr. Tewari and his team delicately remove the cancerous prostate gland while avoiding damage to as many of these nerve bundles as possible.
About fifty percent of men who undergo prostatectomy do experience incontinence immediately after surgery. However, it is short-lived, and for most men this condition resolves quickly (within six months). In fact, 88% of men are pad-free within 6 weeks of surgery; 90% are pad-free within 12 weeks; and 95% are pad-free within a year.
But for others, voiding dysfunction can persist even beyond a year, which may result in both physical discomfort and emotional upheaval due to necessary lifestyle changes.
Our Post-Surgery Rehabilitation Program focuses on providing expert in-office guidance on sexual function, continence, nutrition, exercise, stress management, and alternative medicine options for post-surgical recovery and rehabilitation. Our team comprises qualified medical professionals who are always available to support you post- surgery.

A concern that many men understandably share in considering prostate surgery is what effect it will have on their bladder control.
Dr. Tewari utilizes an anatomic surgical approach that does not involve the use of any thermal (heat) energy which could damage important nerves that control urinary and sexual functioning. This procedure allows for more rapid recovery of continence compared to other surgical methods.
Dr. Tewari's unique technique to preserve continence has gone through several generations of innovations over standard robotic prostatectomy. Each one of these modifications has helped more and more of his patients to ultimately experience no urine leakage or stop urinary leakage sooner after surgery.
Sexual Function After Your Prostate Robotic Surgery
Most of our patients who receive early treatment for prostate cancer, and who had normal sexual function prior to surgery, are able to regain erectile function and enjoy satisfying sex lives after robotic prostatectomy.
However, regaining sexual function is a gradual process and may take up to a year. Very few of our patients experience erectile dysfunction, and we actively work with those who do.
Our Penile Rehabilitation program can play an important role in speeding the ability to resume sexual function. The goal of penile rehabilitation is to keep the penile tissue and muscles oxygenated and stretched to preserve erectile function while the nerves in the penis fully recover.
- Pre-Operative Evaluations:
During your pre-operative visits our experts determine if your particular case could benefit from early evaluations such as penile Doppler studies (a test of blood flow into and out of the penis), and testosterone level estimations. Occasionally we start penile rehabilitation using medications a few weeks before surgery. - Post-operative Rehabilitation:
Post-operative rehabilitation usually starts a few weeks later and may include using intra-urethral suppositories, oral medications, and vacuum device therapies, as well as other approaches to maximize your chances of recovery. We are committed to finding the best option for you.


 International Patients
International Patients